Hemorrhoids or piles occur far more often than you might think. However, considering the stigma surrounding this condition, people often choose not to talk about flare-ups or repetitive cases. Because of this, it’s expected to be more cautious about developing sudden bouts of hemorrhoid symptoms.
To avoid hemorrhoid flare-ups, you’ll need to eat more dietary fiber sources, drink more water, and do Kegel exercises. You must also avoid sitting or standing for a long time, relieve yourself immediately, and avoid straining when doing so. Keep reading to better understand what actions can prevent and treat hemorrhoid flare-ups.
What Causes Hemorrhoids To Flare-Up?
You may find yourself experiencing hemorrhoids only to discover that they were resolved on their own. But then you may experience flare-ups intermittently. And suddenly, you start asking if your hemorrhoids have truly cleared up.
How hemorrhoids form in the first place is yet to be uncovered for clarity. However, several activities have established themselves as apparent triggers for the condition.
In such cases, the same factors cause hemorrhoid flare-ups. According to research, the two things that cause hemorrhoids to flare up are prolonged straining and constipation, which increases abdominal and pelvic pressure. As a result, the veins had to exert too much force in the rectal and anal regions, leading to hemorrhoids.
With this scenario in mind, it’s easier to understand that hemorrhoids don’t occur as a one-time condition. Instead, it could be triggered by the events mentioned above.
Hemorrhoid Self-Care: Avoid Flare-Ups
Although not much is known about how hemorrhoids form, it’s pretty clear that to avoid them, you need to improve your lifestyle and care for yourself on the toilet. The following are tips to follow if you wish to avoid hemorrhoid flare-ups.
- Don’t strain when using the toilet
Straining while you’re pooping accounts for many cases of hemorrhoids. The excess force that pushes your rectum toward the opening causes the veins in your lower anus to swell up.
You may find yourself pushing way too hard on the toilet if you’re experiencing constipation, where you need to excrete hard, dry stool. While this is another issue of its own, the urge to strain can become more apparent, especially if the condition hasn’t improved for an extended time.
However, keep in mind that in doing so, you’ll be simply exchanging one digestive distress with another. If you are constipated, choose to leave the toilet when nothing comes out.
- Avoid prolonged sitting or standing
When you sit for too long, it increases the pressure in the rectal and anal veins. In addition, prolonged standing also impacts blood flow in these areas. Hence, it’s just as bad as sitting for an extended time.
If you wish to avoid hemorrhoid flare-ups, be sure to be more conscious about how long you get into activities requiring you to sit or stand. Be extra cautious with your stay on the toilet. As much as possible, limit your time defecating to avoid straining.
- Add high-fiber foods to your diet
Constipation may cause you to push harder when pooping. Therefore, preventing constipation also helps you avoid hemorrhoid flare-ups by extension. To do this, make sure to fill your diet with high-fiber fruits and vegetables.
Dietary fiber encourages better bowel movement. Not only does eating foods high in fiber move faster in your intestines and make your stool softer, but it also allows for supplementary cleansing, removing debris and buildups on the intestinal walls. On top of that, it aids in weight loss and is a crucial part of renal diets.
- Keep track of your water intake
Aside from increased fiber intake, drinking water regularly also helps in making sure your stool is not too hard to pass. Dehydration or lower fluid intake is a common drive of constipation. This makes perfect sense, as water makes up 75% of fecal matter.
That said, make sure you drink six to eight glasses of water a day or other liquids. Also, consider eating moist or water-rich foods like watermelon, pineapple, oranges, peaches, and celery to reach the recommended daily water intake.
- Don’t hold it in
Delaying your bowels can also spell the worst when it comes to hemorrhoids. For one, this habit promotes constipation, which makes it even harder to push the feces out than it already is when you have a flare-up.
Plus, holding your poop in can also cause tearing in your anal canal (a.k.a anal fissures), which can be associated with hemorrhoids. With that in mind, make sure you’re responding quickly to your urges to defecate.
- Get into Kegel exercises
Kegel exercises strengthen your pelvic floor muscle, which helps regulate the blood flow in the veins affected by hemorrhoids. As a result, it provides additional support and helps reduce hemorrhoid flare-ups.
While Kegel exercises are popular among women, men can perform them thrice daily. This is in addition to other exercises that improve your cardiovascular functions, such as walking, cycling, and even light physical activities you can do at home.
When to See a Doctor About Your Hemorrhoid Flare-Up

Schedule an appointment with your doctor if the symptoms persist for weeks and begin to worsen despite treatment. More so, if you observe any rectal bleeding, which can be a hemorrhoid flare-up symptom but can also indicate other conditions like diverticulitis, polyps, Crohn’s disease, and colorectal cancer.
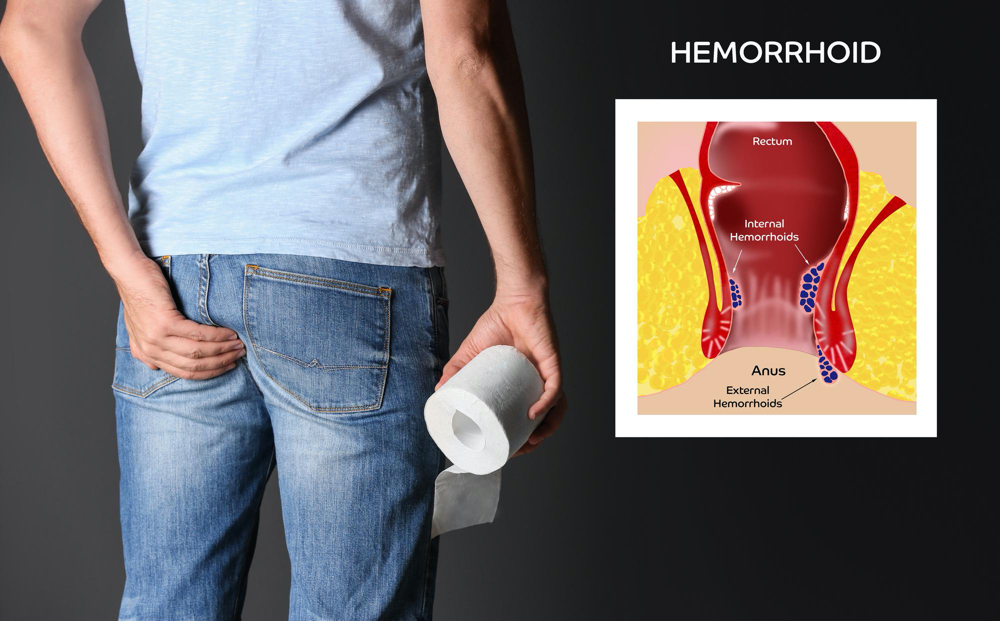
Hemorrhoids can be internal or external. External hemorrhoids affect the anal region with symptoms such as pain, itching, and hard lumps around the anus.
On the other hand, internal hemorrhoids develop in the rectum. It typically has no symptoms but can also cause bleeding from inside the affected tissue.
To diagnose hemorrhoids, doctors often perform a physical exam to check for lumps. In the case of internal hemorrhoids, a fecal occult blood test may be requested, and perhaps other tests to rule out other causes of the bleeding.
Frequently Asked Questions
How long do hemorrhoid flare-ups last?
Hemorrhoid flare-ups usually last between 2-7 days or even longer than that, depending on how severe the condition is and the type of treatment applied. Several instances show that it can last for 2-3 weeks. Keep in mind that if the hemorrhoids don’t heal even after the medications and hemorrhoids self-care, consulting your doctor is the way to go. You may need to have it surgically removed, depending on clinical recommendations.
Does a hemorrhoid flare-up go away on its own?
It’s possible for a hemorrhoid flare-up to get rid of itself within a few days (often within or less than a week), even without medications. This is more common in mild cases and if home remedies were applied to relieve hemorrhoid flare-up symptoms.
On the other hand, chronic hemorrhoids may not clear up without proper treatment. Check with your doctor to ensure you get an accurate sense of your hemorrhoid’s severity.
What is the fastest way to heal a hemorrhoid?
You can relieve external hemorrhoid flare-ups by applying hemorrhoid creams or using a suppository. These medications can be purchased over the counter and typically contains hydrocortisone for rectal inflammation. However, if you still experience flare-ups even after application, consult your doctor and better halt the use of the said treatment.
On top of this, consider applying a numbing pad or wipes with witch hazel or ice pad for a short time. Also, soak in a warm bath or sitz bath for 10 to 15 minutes about three times a day.
The Bottom Line
Hemorrhoids cause pain and extreme discomfort that could disrupt your daily schedule. But you can avoid these flare-ups or at least reduce their impacts by becoming more conscious about your diet, exercise, and toilet activity. Doing the above mentioned tips for hemorrhoid self-care increases your chance of preventing any complications that need surgical procedures.
Related Articles
